Colorado Preferred Network
Participating Provider Resources
No obligation level of care crisis assessments via walk-in, by appointment, telephone or telehealth. Acute psychiatric stabilization for individuals in behavioral health crisis.
Psychiatric hospitalization for adolescents 12-17 years and adults 18+ years; medical detox for adults 18+ years offering withdrawal management from alcohol, benzodiazepines, polysubstance use.
30 hours per week (Monday-Friday) of group-based therapy with medication evaluation and management. Programs for: adolescents (12-17), adults, active duty military, veterans, first responders, and other occupations with high-risk trauma exposure.
3 days per week/3 hours per day (total 9 hours per week) of group-based therapy. Specialties include adolescents age 12-17; mental wellness; chemical dependency, caregivers, and faith/spiritual based.
Telepsychiatry allows patients to see a psychiatric provider over easy and accessible video. Our psychiatric providers practice across all specialties, ages and acuity levels.
Follow-Up After Hospitalization provides post-discharge psychiatric appointments within 7 days. FUH, a care quality measurement score, is emerging as a critical tool for closing care gaps and decreasing readmission.
We match clients with licensed specialists for in-person or video therapy sessions in order to seamlessly continue treatment as directed by a referring provider. If preferred, therapy can also be directed at the discretion of our matched therapist.

Tackling the biggest challenges in behavioral health care delivery
Behavioral health care is complex and you see it every day. You are doing your best to care for patients but the system is fragmented; however it can be difficult to get referral appointments, and some patients need coordination of care that you cannot easily provide.
Optum is piloting a new preferred network to help you with those challenges.
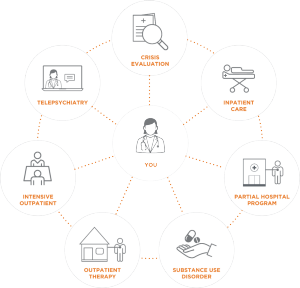
Transforming Behavioral Health Care Delivery
As a member of our preferred Colorado network pilot, you and your patients have access to a wide range of resources that will accelerate treatment, improve outcomes, and deliver coordinated care. You will have:
Accelerated Access: Providers in our preferred network have been pre-selected as high-quality practitioners who are available for referrals and will serve your patients’ needs in less time. If your patient needs services like medication management, crisis support or self-support tools they will be readily available.
Measurement-Based Quality: You will have access to the patient reported outcomes tools needed to deliver high-quality measurement-based care.
Clinical Guidelines: Our preferred network partners have worked together to provide clear guidelines regarding how to triage your patients to the right level of care.
Integrated Care Coordination: Our staff of trained care coordinators will help you get your patient to their appropriate level of care, make their appointments, and continue their ongoing care with you as needed.


